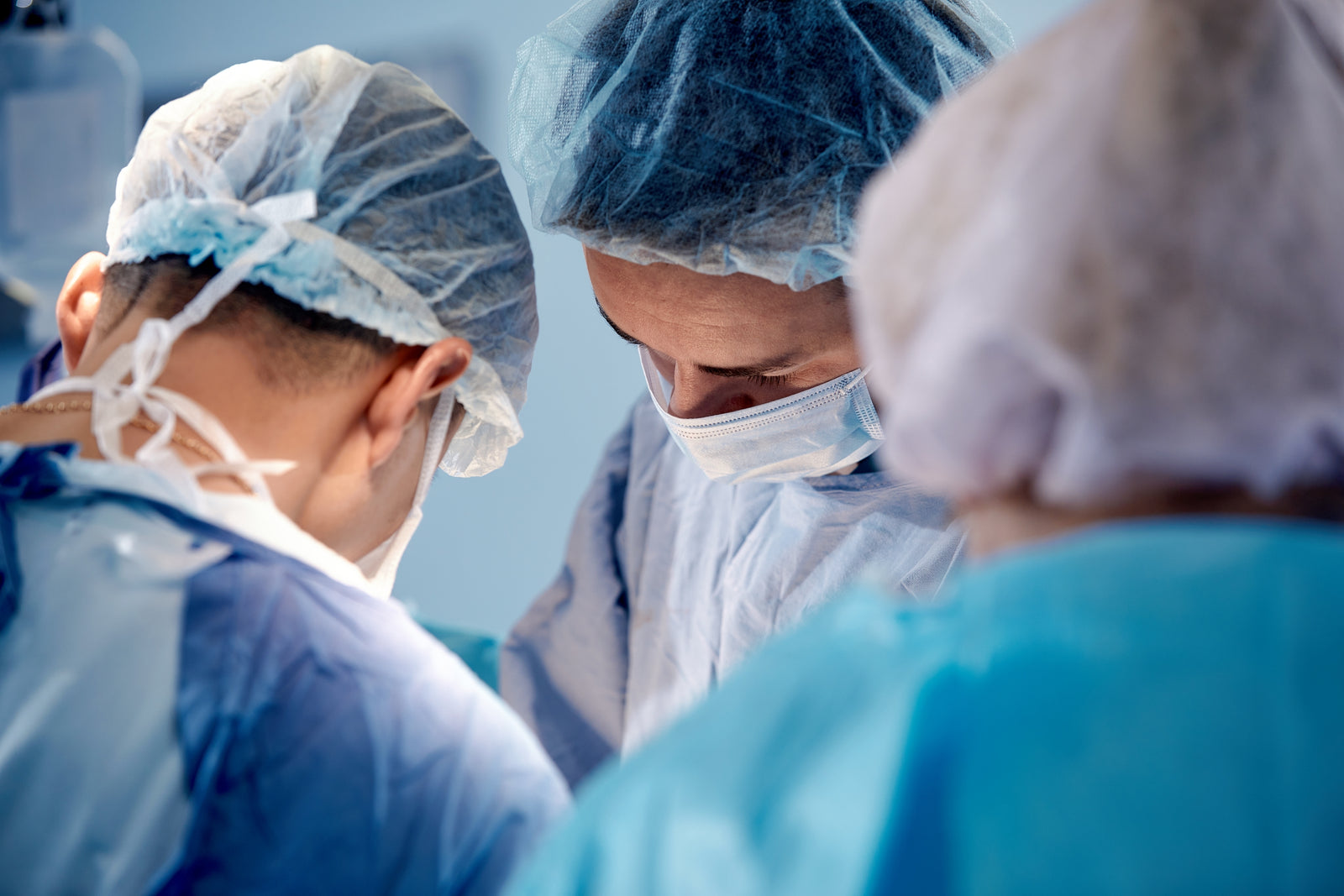
The issue of medical device contamination is becoming more widely recognized as a leading cause of device failure—and many researchers now acknowledge that the number of patients affected globally by medical device-related infections has been grossly underestimated.
Device contamination has a major impact on patient care. Complications are serious, ranging from restricted mobility and mild to severe pain (at best) to the need for revisional surgery or amputation, and even death. Numerous studies have shown that between 70-100% of explanted hardware from failed joint implants have some level of contamination.*
A long list of operating-room safety protocols are employed to minimize the risk of patient infection. Among these widely-adopted surgical sterility precautions include education and training for medical professionals, PPE use, double gloving, routine glove changes, safe injection and medication management, environmental cleaning and disinfection; and the cleaning, disinfecting and sterilization of medical instruments and devices. Despite these extensive efforts, most operating rooms and surgical suites are rife with bacteria, making implant failures and infections a tremendous risk for patients.
Even with the strictest diligence of operating room staff, bacteria can also be introduced by the airflow system or the staff in the operating room itself. Alarmingly, studies reveal that up to 70% of the bacteria from the air can land on sterile surfaces such as surgical instruments and implants and be transferred to the patient wound site. Studies have also shown that the longer surgical instruments or implants are exposed to the air in the operating room, the greater the likelihood of contamination that can lead to surgical site infection.**
Bacteria by themselves are usually killed by our immune systems. Without an implant, it can take up to 100,000,000 bacteria to cause an infection. With an implant (even from a sterile package), as few as 100 bacteria can cause an infection. When medical device bacterial infection occurs, it is 10,000 times more likely to lead to sepsis as compared to injecting bacteria into the bloodstream—and there is no definitive evidence that blood-borne infections can lead to implant contamination.
So why does the device contamination problem persist—and continue to grow?
Because current operating room protocols designed to reduce bacterial contamination during surgery only indirectly protect the implant surface. Since we’ve learned that it’s almost impossible to completely eradicate contamination and resulting infections, it makes sense that every implant should have some antibacterial protection.
Orthobond is the first company to utilize surface modifications that can be permanently bound to any metal or polymer medical-implant surface. The company’s Ostaguard technology kills bacteria by mechanically rupturing pathogens—and without the use of antibiotics.
Orthobond’s proprietary antibacterial technology makes it uniquely positioned to solve one of the world’s largest healthcare challenges, as contaminated implant devices lead to thousands of hospital-acquired infections every year. We believe our science is a big step forward for a community that has been waiting on major innovation for decades—and that it will make an immediate difference for those performing and undergoing surgeries.
_________________________



